

A cornea is a transparent component of an eye that covers the pupil, iris, and anterior chamber of the eyes. The cornea protects the inside part of an eye, it refracts the light and focuses light on the retina. The cornea should be smooth, clear, and healthy to function properly. The damaged cornea becomes swollen and scarred due to which it cannot focus the light properly onto the retina, and as a result, your vision will be compromised. So you will see all blurry vision.
If the damage is small, then it can heal itself. However, the major damage can not heal itself and you may need transplantation of the cornea. A cornea transplant surgery in India involves replacing the damaged cornea with a healthy one retrieved from healthy donor tissue. For patients exploring options for cornea transplant in india, CureIndia connects you with internationally trained ophthalmologists and top-ranked eye hospitals that offer premium care at highly affordable prices. Patients comparing the eye transplant cost in india against western benchmarks consistently find savings of 70–80%, making India the most sought-after destination for corneal graft surgery worldwide.
Cornea disease is one of the leading causes of blindness worldwide. A cornea transplant is also known as keratoplasty. It is a surgical procedure in which the diseased cornea of a patient’s eye is removed. Then, it is replaced by the donor cornea tissue. While this procedure is widely available in developed countries, many developing countries still need a long way. For example, there is a shortage of donor corneal graft tissues in both the private as well as public healthcare sectors.
In Africa, they have to import donor corneas from other countries. The African nations greatly rely on the USA to supply the donor cornea to their country. For the majority of African people, the cost of these imported donor corneas is unaffordable due to which they don’t receive the treatment on time and have to stay on a long waiting list.
It is due to this reason that many Africans from countries like Ethiopia, Cameroon, Kenya, Tanzania, and Zambia travel to India every year for cornea transplant surgery. The donor cornea graft tissue is widely available in India and the medical procedure is smooth from the start till the end.
Due to advanced medical technologies and highly experienced eye specialists, Eye hospitals in India can provide premium treatments and comfortable medical care. In addition, eye treatments are budget-friendly and reliable in India. Many people from across the globe are visiting India for world-class treatments at a much cheaper cost.
The cornea transplant surgery in India restores the impaired vision due to the damaged cornea. The transplantation of the cornea also relieves pain and other symptoms associated with a damaged cornea. Many eye conditions can be treated by corneal graft transplant; a few of them are listed below. Choosing cornea transplant in india is particularly beneficial for patients from Africa and other developing regions where donor tissue is scarce and the same procedure costs significantly more.
■ Keratoconus: In this eye disease, the cornea becomes thin. It starts bulging out and forms a cone shape. This can cause vision problems and sensitivity to light and glare.
■ Fuchs’ dystrophy: It is an eye disease in which the cornea increases in thickness. It causes visual impairment. In this disease, the innermost layer of the cornea (known as corneal epithelium) removes the fluid from the cornea. It stops functioning as the cells die.
■ Corneal Ulcer: It is an eye disease in which the cornea becomes infected, causing redness in the eye because blood vessels become swollen, making the eye watery. It causes severe pain in the eyes and often causes pus and other eye discharge. It leads to loss of vision and blindness.
■ Bullous Keratopathy: It is an eye disease in which the cornea becomes swollen due to infection or injury that damages the innermost cornea layer.
There are three different options for a cornea transplant surgery in India. The cornea is made up of three layers. Depending upon the patient’s need, these three surgeries are designed to target the specific layer of the cornea.

It is important to note that the cornea graft tissue is donated by deceased human donors. Hence, they are known as donor cornea graft tissue. Before the procedure, these donor corneas undergo testing to make sure that it are suitable and safe for the patient and transplant, respectively. The three corneal graft transplant surgeries are mentioned below.
It is also known as full-thickness cornea graft transplantation. In this procedure, the surgeon removes the centre part of the diseased cornea with the help of a small circular blade. After removing it, the surgeon then replaces it with a healthy piece of donor cornea.
This is a surgical procedure used to remove the back tissues (innermost layer) of the corneal layers. It consists of endothelium and Descemet membrane. There are two types of endothelial keratoplasty, namely. In Descemet stripping endothelial keratoplasty (DSEK), the donor corneal tissues replace one-third of the cornea, and in Descemet Membrane Endothelial Keratoplasty (DMEK), a thinner layer of the donor’s cornea is used to replace the diseased corneal tissues.
This is a surgical procedure in which the middle and outer (front) layer of the damaged cornea is replaced by the donor corneal tissue. It is sometimes also known as Deep Anterior Lamellar Keratoplasty (DALK) or Partial Thickness Corneal Graft Transplant. It is commonly used for the treatment of a bulging cornea disease known as keratoconus.
If for some reason you don’t get the right donor, or if you are not eligible to receive a donor cornea for your cornea transplant surgery in India, then an artificial cornea, which is made up of transparent polymers, can be used to replace a diseased cornea. This is a surgical procedure known as keratoprosthesis. Patients who wish to understand what type of cornea transplant in india suits their specific eye condition can consult with CureIndia's partner ophthalmologists for a personalised evaluation before confirming their travel dates.
Before deciding on the surgery date, your doctor will discuss a few things as to why you need the cornea transplant surgery in India. The doctor will discuss the cornea transplant procedure, recovery, results, etc. Once everything is clear between the doctor and the patient, the surgery day will be fixed. It is necessary to inform your doctors about all the medications you are taking for any existing medical condition.

On the day of the procedure, the surgery will proceed by first giving you a sedative to keep you calm and local anaesthesia to prevent pain during the surgery. The surgeon will use a microscope to perform the surgery. A medical device will keep your eye open during the operation.
Depending upon what part of the cornea is to be replaced, your surgeon will remove the diseased cornea and replace it with the new cornea donated by a donor. The donor corneal tissue is then sutured with an ultra-fine thread. It will remain in place until your eye recovers and heals completely. Once the eye is healed, the thread is removed by the surgeon easily.
If you have any other eye problems and need surgical intervention to repair and treat them, then it will also be performed during this same operation. Many times the cataract surgery is performed along with cornea repair surgery. Once the replacement is done, the patient’s eyes will be covered with the eye patch to keep the eye safe and shielded. The patient will be kept under observation until the anaesthesia wears off.
Once the anaesthesia wears off, the patient can go home with a family member on the same day of their cornea transplant surgery in India. The patient is suggested to arrive for an after-surgery check-up. Depending upon the rate at which your eye heals, the stitches are removed the next day or after a few days.
You will be given some instructions to follow after the cornea transplant surgery in India. Make sure that your eyes remain safe, and it starts to heal. Your ophthalmologist will prescribe some eye drops. You should be careful and avoid rubbing your eyes, and you need to wear an eye shield or eyeglasses to keep your eyes protected. You might need to lie down on your back for a while after the surgery to help the new cornea tissue stay in place.

CureIndia is a platform where we help people choose the right eye hospital and eye specialist for medical treatments. The doctors in our associated eye hospitals are internationally trained and highly experienced. The majority of them are active members of many international medical councils and associations. Let’s hear from some of our most reputed cornea transplant doctors in India.




The total cornea transplant cost in India is influenced by many factors such as the type of transplant needed, the patient’s health and age, hospital, medication cost, travel cost, insurance coverage, etc. However, the average cornea transplant cost in India can range from 1,500 USD to 2,000 USD per eye. Note that the price of that can vary a little in different cities in India. As there are different types of cornea replacement surgery in India, the average cost of the different cornea replacement surgery types is listed below.
| Treatment | Cost in India | Stay in India |
|---|---|---|
| Cornea Transplant Surgery in India | $2,000 per eye | 5-7 days |
| Artificial Cornea Transplant Surgery in India | $3,000 per eye | 5-7 days |
The cost of cornea replacement surgery in the USA ranges from 13,000 USD to 27,000 USD, and in the UK it can cost around 11,300 USD. As we can see, the cost of this treatment is much lower in India as compared to developed countries like the USA and the UK.
The treatment services are the same in all of the countries, namely India, the United States, and the United Kingdom, but there is a big difference in the cost of the treatments. This is because the travel cost is much cheaper in India. People can receive high-quality treatments at a very low cost. A lot of people from across the world are choosing India for various medical treatments. Patients who have already compared the cornea transplant cost in india against USA and UK prices understand that choosing India through CureIndia offers both significant financial savings and access to the same internationally certified surgical standards.
Cornea transplant surgery in India is a surgery that can help people improve their vision and heal from the trauma. The damage is caused to the cornea of an eye due to injury or infection. This surgery is widely available in developed countries, whereas many low-income countries don’t have enough medical resources to provide an effective treatment.
The cornea surgery requires a donor cornea tissue to replace the patient’s damaged cornea. Many countries don’t have enough donors, and that’s why they have to import donor corneal graft tissue from other countries. This makes the treatment very expensive, which is not affordable for many patients. Due to this, not many people can receive the treatment, and their eye condition becomes worse.
That is why a lot of people from these countries travel to India for their eye treatment. As the treatment in the top cornea transplant hospitals in India is of premium quality and is much cheaper, people travelling from other nations to India can have a profitable option for their cornea transplant surgery in India. This is highly beneficial for them, as they not only receive the correct treatment but also save a lot of money by choosing India. The eye transplant cost in india combined with CureIndia's all-inclusive medical travel support, covering airport transfers, hotel accommodation, and dedicated case managers, makes India the most complete and cost-effective destination for corneal graft surgery globally.


Get the Eye color you've always dreamed of
Connect Today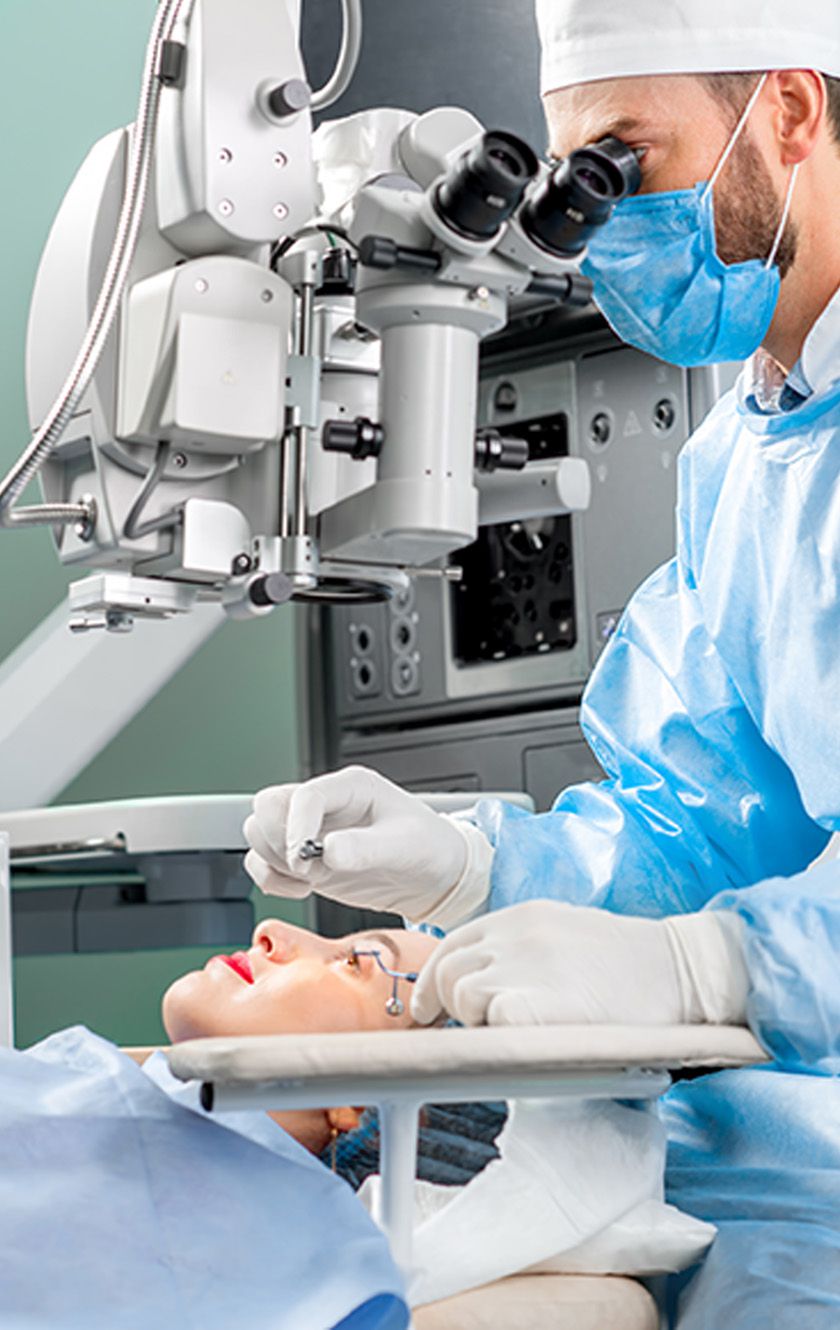
Opt for successful eye color change surgery
Plan Surgery
Remove glasses with SMILE LASIK
Get Cost